What is Lipoprotein (a) and why do we need to measure?
By Dr Rohit Khurana
What is Lipoprotein (a)
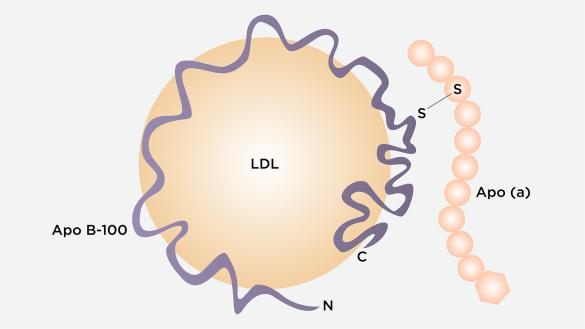
Lipoprotein (a) [Lp (a)] is a low density lipoprotein (LDL) particle with an added apolipoprotein(a), which is bound covalently to the apoB contained in the outer shell of the particle. It is made in the liver and measured in the blood plasma.
Plasma levels of Lp(a) depend on the size of the apolipoprotein (a) isoforms which explain most of the variability seen in different populations and ethnic groups. An individual's Lp(a) level is 80-90% genetically determined in an autosomal codominant inheritance pattern with full expression by 1-2 years of age and adult-like levels achieved by approximately 5 years of age. Outside of acute inflammatory states, the Lp(a) level remains stable through an individual's lifetime regardless of lifestyle.
High levels of Lp(a) have now been identified as an independent risk factor in cardiovascular disease, even when cholesterol levels and other classical risk factors such as elevated cholesterol, hypertension and diabetes have been taken into account. Lp(a) has a causal link to atherosclerosis (which blocks arteries) and increasing the tendency for the blood to clot.
Who should be Screened for Lp (a)?
Current recommendations from the European Atherosclerosis Society (EAS) are to screen people who are at intermediate, moderate or high risk of developing cardiovascular disease. This should include those with premature cardiovascular disease, a family history of premature cardiovascular disease, family history of elevated Lp(a), familial hypercholesterolaemia (FH) and those with recurrent cardiovascular disease despite optimum medical treatment.
Most people have Lp(a) levels in the range of <30mg/dl. Based on the available studies, the guideline recommends a universal cut off point ≥ 50 mg/dL, which approximates the 80th percentile in the Caucasian U.S. populations. Once levels of Lp(a) have been determined, they do not usually need to be checked again, but it is important to continually monitor the other identified risk factors.
How do you treat Lp (a)?
The optimal way to treat elevated Lp(a) is still under investigation. Currently the most important management strategy for people with high levels of Lp (a) is to optimise/treat all other modifiable risk factors, in particular LDL cholesterol. The best treatment for Lp(a) is to reduce the cholesterol burden of the particle with a statin which will shrink the particle size. Other treatments shown to help lower Lp(a) levels include PCSK9 inhibitors (reduce levels by 25%). Co-enzyme Q-10 and fish oils have been suggested as beneficial but have not been proven in clinical trials. A new injectable treatment known as an anti-sense therapy which stops Lp(a) being made is nearing the end of Phase 3 clinical trials. Work so far has shown this treatment can reduce Lp(a) levels by up to 90% making this approach a potentially new and additive component to primary and secondary prevention of heart disease.

